
Jaliyah Robinson
Jacksonville State University
NU 390
Dr. Stacey Mikel
April 17, 2026
This e-portfolio explores the phenomenon of alert fatigue occurring in the practice of nursing. The rising numbers of clinical decision support (CDS) alerts within the growing complexity of the electronic health record (EHR) have the potential to improve patient safety. However, many of these alerts are overused, over warnings are produced, and the alerts are often nonspecific, leading to fatigue of the alert. Additionally, the alerts can interfere with the clinical workflow and can lead to errors. Recent research highlights that repeated exposure to frequent alerts leads to cognitive overload and decreased responsiveness, ultimately compromising patient safety and care quality (Michels et al., 2025; Salameh et al., 2024). This project investigates the causes of alert fatigue based on system design and workflow inefficiencies and develops evidence-based interventions to increase the effectiveness of clinical alerts with the ultimate goal of promoting patient safety. In addition to supporting high-stake clinical decision-making, improving nursing workflow and effective use of informatics is a critical aim of this project.
Issue Analysis
Alert fatigue is a phenomenon in which repeated exposure to excessive or irrelevant clinical alerts leads to desensitization and delayed or missed responses by healthcare providers (Michels et al., 2025). Nurses in today’s hospitals may receive hundreds of alerts each shift, only a small percentage of which are clinically relevant and require action. The high volume of alerts can create a hazardous environment in which patients’ needs are endangered by being submerged by irrelevant information.

Clinical Impact & Stakeholders
Alarms and alerts are ubiquitous in modern healthcare but alerts that are not pertinent to the specific care scenario presented by a patient can lead to alert fatigue – a list of dangers that includes increased risk of medication error, delayed recognition of a patient’s deterioration, and cognitive overload or stress, all resulting in decreased nurse effectiveness and increased nurse burnout. Furthermore, unreliable or inaccurate clinical decision support systems (CDS) can lead to decreased trust in these systems among clinicians.
Studies show that alarm fatigue contributes to delayed or inadequate responses, ultimately compromising patient safety and care quality (Michels et al., 2025; Salameh et al., 2024).
Additionally, nurses exposed to frequent alarms report higher stress levels and workload burden, further impacting performance and patient outcomes (Salameh et al., 2024).
Stakeholders include nurses, physicians, patients, & IT developers/professionals.
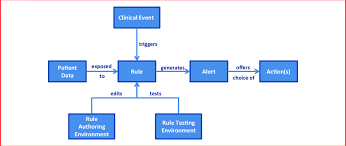
- Nurse enters patient data into EHR
- CDS system generates multiple alerts
- Alerts interrupt workflow
- Nurse overrides or ignores alerts
- Critical alert may be missed → Patient safety risk!!!

Analysis
Current CDS systems are primarily developed around mode of intervention of alerts (i.e., interruptive vs. non-interruptive) with little emphasis on prioritization or clinical context. Furthermore, most CDS rules do not take into consideration the relevant patient data; as a result, a large volume of unnecessary and repetitive alerts are generated for clinicians treating individual patients.
Alert fatigue and clinical alarm disturbance were greatest patient safety concerns. Contributing factors to these issues included high volume of non-actionable alerts, poor alert prioritization, lack of patient specific customization, lack of nurse involvement in system design, and lack of adequate usability testing.
Research shows that excessive alert burden reduces system effectiveness and contributes to alert fatigue, ultimately decreasing clinician responsiveness (Thompson et al., 2024).
Recommendations
1. Implement Tiered Alert Systems
Create an alert system that separates between high, medium, and low priority.
Why It Works:
Helps reduce user cognitive overload and brings attention to critical alerts.
Evidence:
Excessive alerts are a primary driver of alert fatigue, and reducing alert volume improves response rates (Michels et al., 2025).
2. Improve Alert Specificity Using Patient Data
Simulate patient specific data that incorporates diagnosis, medications, and medical history.
Why It Works:
Irrelevant alerts are reduced and clinical relevance is improved.
Evidence:
Optimizing CDS systems to reduce unnecessary alerts is essential to minimizing alert burden and improving usability (Thompson et al., 2024).
3. Increase Nurse Involvement in System Design
Involve bedside nurses into the development of CDS evaluation.
Why It Works:
This ensures that real time clinical workflows are reflected.
Evidence:
Human-centered design improves system effectiveness and reduces workflow disruption (Michels et al., 2025).


Recommendations
4. Provide Ongoing Training & Education
Ensure that nurses prioritize and recognize critical alerts.
Why It Works:
This reduces override alerts that are inappropriate and guides appropriate clinical decision making.
Evidence:
Knowledge gaps contribute to poor alarm management and ineffective responses (Journal of Emergency Nursing study, 2025).
5. Continuous Monitoring & Quality Improvement
Monitor the rates at which track alerts are overridden and continually refine CDS systems in order to increase their effectiveness
Why It Works:
This increases and ensures effectiveness in the systems that is long term.
Evidence:
Ongoing evaluation is necessary to manage alert burden and maintain safety (Thompson et al., 2024).
Alignments with Nursing Informatics Best Practices
These solutions align with informatics competencies by:
- Enhancing patient safety and quality outcomes
- Supporting evidence-based practice
- Promoting user-centered design
- Improving workflow efficiency
- Utilizing data-driven decision-making
This reflects the nurse’s role in identifying system inefficiencies and implementing informatics solutions to improve care delivery.

References
Agency for Healthcare Research and Quality. (2024). Alert fatigue.
Emergency Nurses’ Knowledge Study. (2025). Journal of Emergency Nursing. https://doi.org/10.1016/j.jen.2024.11.007
Michels, E. A. M., Gilbert, S., Koval, I., & Wekenborg, M. K. (2025). Alarm fatigue in healthcare: A scoping review. BMC Nursing, 24, 664. https://doi.org/10.1186/s12912-025-03369-2
Salameh, B., Abdallah, J., & Alkubati, S. (2024). Alarm fatigue and perceived stress among ICU nurses. BMC Nursing, 23, 261. https://doi.org/10.1186/s12912-024-01897-x
Thompson, S. A., Kandaswamy, S., & Orenstein, E. (2024). Reducing nursing alert burden. Applied Clinical Informatics, 15(4), 727–732. https://doi.org/10.1055/a-2345-6475
For this assignment’s preparation, the author utilized ChatGPT, a language model created by OpenAI. Within this assignment, ChatGPT was used for brainstorming & structuring content for the creation of this website.